Laparoscopy & Hysteroscopy in Chennai
Minimally invasive laparoscopy and hysteroscopy in Chennai to diagnose and treat conditions affecting fertility — with faster recovery and better reproductive outcomes.
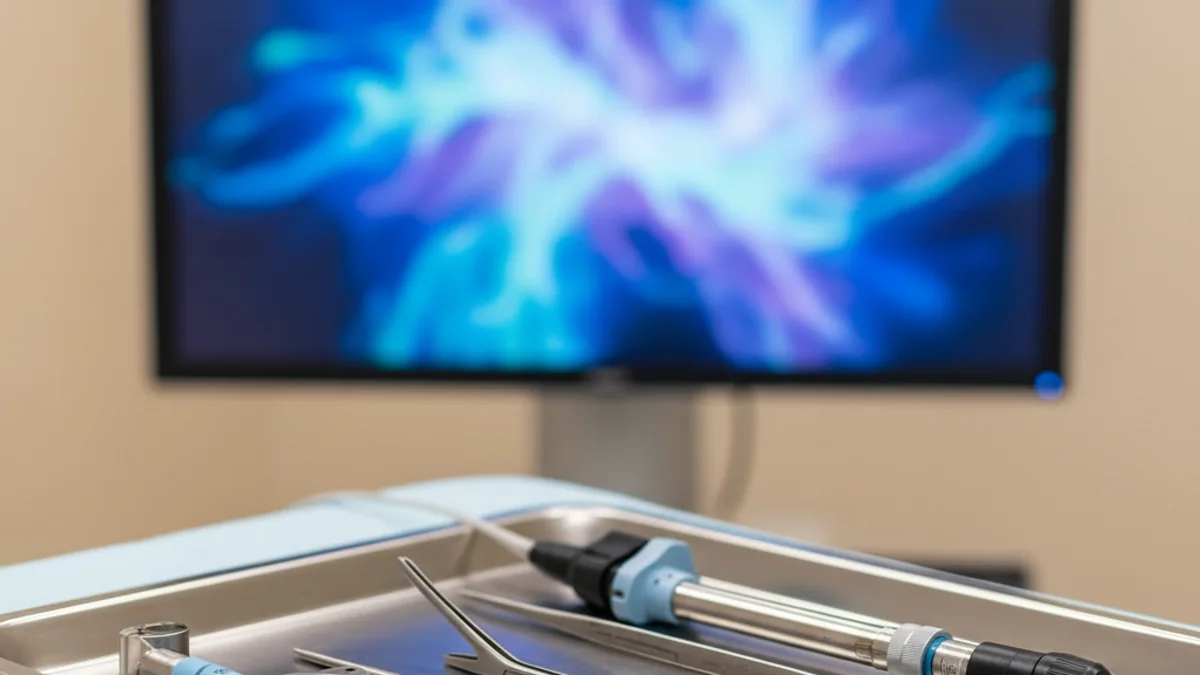
Gynecological endoscopy — encompassing both laparoscopy and hysteroscopy — has transformed how conditions such as endometriosis, fibroids, ovarian cysts, and tubal blockages are diagnosed and treated. For women experiencing infertility, these minimally invasive procedures often uncover and correct problems that cannot be detected through imaging alone, removing barriers to conception without the prolonged recovery associated with open surgery. Dr. Rukkayal is trained in advanced endoscopic techniques and integrates these procedures into a comprehensive fertility treatment plan, ensuring that surgical findings directly inform your next steps toward pregnancy.
Laparoscopy involves small incisions through which a camera and specialised instruments are inserted into the abdominal cavity, allowing direct visualisation and treatment of conditions affecting the uterus, fallopian tubes, and ovaries. Hysteroscopy accesses the uterine cavity through the cervix — no abdominal incisions at all — to evaluate and treat polyps, fibroids, adhesions, and structural anomalies within the womb. In many cases, diagnosis and treatment happen simultaneously during the same procedure, avoiding the need for a second surgery. The minimally invasive nature of these approaches means smaller incisions, significantly less post-operative pain, shorter hospital stays (often same-day discharge), and faster return to normal activities and fertility treatment. For women planning IVF, addressing conditions like endometriosis or uterine polyps before embryo transfer can meaningfully improve implantation and pregnancy rates.
1500+
Endoscopic Procedures
60-70%
Post-Surgery Conception Rate
When Is Diagnostic or Operative Endoscopy Recommended?
You should see a specialist if you experience:
- Unexplained infertility despite normal initial investigations
- Suspected endometriosis based on symptoms or imaging
- Recurrent IVF failure suggesting a uterine cavity issue
- Abnormal uterine bleeding or suspected polyps or fibroids
- Blocked fallopian tubes identified on HSG
- Suspected uterine adhesions or structural anomalies
Understanding Gynecological Endoscopy
Laparoscopy and hysteroscopy are complementary procedures that together provide complete evaluation of the reproductive tract. Laparoscopy examines the external surfaces of the uterus, fallopian tubes, and ovaries, as well as the surrounding pelvic anatomy. It is the reference standard for diagnosing endometriosis, assessing tubal patency, removing ovarian cysts, and treating adhesions that distort normal anatomy. Hysteroscopy focuses on the inside of the uterus — the cavity where embryo implantation occurs. It identifies and treats polyps, submucosal fibroids, intrauterine adhesions (Asherman syndrome), and uterine septae that can interfere with conception or increase miscarriage risk. Both procedures use high-definition cameras and specialised instruments that allow precise work through incisions of five to ten millimetres or no incisions at all. The minimally invasive approach preserves surrounding healthy tissue, reduces blood loss, and allows most patients to resume daily activities within three to five days — a fraction of the recovery time required after traditional open surgery.
Conditions We Treat with Endoscopy
Our Endoscopic Procedures
Diagnostic Laparoscopy
A camera-guided examination of the pelvic organs to identify endometriosis, adhesions, tubal damage, or other conditions that may not be visible on imaging. Often combined with dye testing (chromopertubation) to assess whether the fallopian tubes are open.
Operative Laparoscopy
Treatment performed during the same procedure — excision or ablation of endometriosis, removal of ovarian cysts (cystectomy), adhesiolysis, and management of ectopic pregnancy, all through small keyhole incisions.
Laparoscopic Myomectomy
Minimally invasive removal of uterine fibroids that may be distorting the uterine cavity or affecting blood supply to the endometrium, improving the environment for embryo implantation.
Diagnostic Hysteroscopy
A slender camera is passed through the cervix to directly visualise the uterine cavity, identifying polyps, fibroids, adhesions, or structural anomalies that standard ultrasound may miss.
Operative Hysteroscopy
Removal of polyps (polypectomy), submucosal fibroids, intrauterine adhesions, or correction of a uterine septum — all performed through the cervix with no abdominal incisions and typically same-day discharge.
Why Choose Dr. Rukkayal?
- Advanced endoscopic training with MRCOG (UK) and extensive hands-on surgical experience.
- Integrated fertility-focused approach — surgical findings directly guide your IVF or IUI treatment plan.
- Simultaneous diagnosis and treatment in a single procedure, avoiding the need for repeat surgeries.
- Minimally invasive techniques that preserve ovarian tissue and reproductive potential.
- Same-day or next-day discharge for most endoscopic procedures.
- Clear, honest pre-operative counselling so you understand exactly what to expect and why the procedure is recommended.
- Convenient locations across Chennai — Egmore/Chetpet (morning), Mylapore (evening), and Tambaram — plus visiting consultant at Apollo, Motherhood & Cloudnine hospitals.
Your Treatment Journey
Pre-Surgical Evaluation
A thorough review of your imaging, fertility history, and symptoms to determine whether laparoscopy, hysteroscopy, or both are indicated. Pre-operative blood tests and anaesthesia fitness assessment are completed.
Procedure Day
The procedure is performed under general anaesthesia in a fully equipped operating theatre. Laparoscopy uses two to three small incisions (5-10 mm); hysteroscopy requires no incisions. Both typically take 30 to 90 minutes depending on findings.
Intraoperative Findings & Treatment
Conditions identified during the procedure are treated in the same sitting wherever possible — endometriosis excision, cyst removal, polyp removal, adhesion release, or tubal assessment with dye testing.
Recovery & Discharge
Most patients are discharged the same day or the following morning. Post-operative pain is typically mild and managed with oral medication. Detailed recovery instructions and a follow-up appointment are provided before discharge.
Follow-Up & Fertility Planning
A follow-up visit at one to two weeks reviews surgical findings, histopathology results (if tissue was sent), and outlines the next steps in your fertility treatment — whether that is natural conception, IUI, or IVF.

Have Questions About Your Treatment?
Book a consultation with Dr. Rukkayal Fathima to understand your options and next steps.
Frequently Asked Questions
Yes. Laparoscopic excision of endometriosis — particularly when it involves the ovaries (endometriomas) or distorts tubal and pelvic anatomy — has been shown to improve natural conception rates and IVF outcomes. The extent of improvement depends on the stage and location of endometriosis, which Dr. Rukkayal will discuss with you based on intraoperative findings.
Most patients can resume fertility treatment within one to two menstrual cycles after laparoscopy. In some cases, particularly after minor procedures like polyp removal via hysteroscopy, treatment can resume in the very next cycle. The timeline is individualised based on the procedure performed and your recovery.
Hysteroscopy and straightforward diagnostic laparoscopy are typically day-care procedures with same-day discharge. More extensive operative laparoscopy (such as large cyst removal or advanced endometriosis excision) may require an overnight stay for observation. You will know the expected plan before your procedure.
Yes. During laparoscopy, a coloured dye is passed through the uterus and tubes (chromopertubation). If the dye spills freely from the ends of the tubes, they are confirmed as open. This is considered more accurate than an HSG (hysterosalpingography) X-ray test and has the advantage of allowing treatment if a problem is found.
Not all fibroids require removal before IVF. Submucosal fibroids (those growing into the uterine cavity) and large intramural fibroids that distort the cavity are the types most likely to affect implantation and should be removed. Smaller fibroids that do not distort the cavity are usually monitored rather than surgically addressed. Dr. Rukkayal will review your specific scan findings to advise accordingly.
Recovery after hysteroscopy is rapid since there are no abdominal incisions. Most women experience mild cramping for a few hours and light spotting for one to two days. You can typically return to normal activities within 24 to 48 hours. Strenuous exercise is best avoided for about a week.
Yes. Intrauterine adhesions (Asherman syndrome) are one of the primary indications for operative hysteroscopy. The adhesions are carefully divided under direct vision, restoring the normal shape and lining of the uterine cavity. Post-procedure, a short course of oestrogen therapy is often prescribed to promote healthy endometrial regeneration.
For most ovarian cysts encountered in fertility patients, laparoscopy is the preferred approach. It offers smaller incisions, less post-operative pain, shorter hospital stay, faster recovery, and importantly, better preservation of healthy ovarian tissue — which is critical when future fertility is a consideration. Open surgery is reserved for very large cysts or suspected malignancy.
Yes, combining laparoscopy and hysteroscopy in a single session under one anaesthesia is a common and efficient approach. This allows Dr. Rukkayal to evaluate the external pelvic anatomy and the internal uterine cavity in the same procedure, providing a complete picture of your reproductive tract without the need for two separate surgeries. The combined approach is particularly useful when both tubal assessment and uterine cavity evaluation are needed as part of a fertility workup.
In many cases, the post-operative fertility window is one of the best times to try conceiving. After procedures such as endometriosis excision, adhesion removal, or tubal treatment, natural conception rates are typically highest within the first 3 to 6 months following surgery. Dr. Rukkayal will advise you on the ideal timing based on your specific procedure and recovery, and may recommend starting fertility treatment such as IUI or IVF within this window to take advantage of the improved pelvic environment.
Related Specialties
Hysteroscopy Treatment
Direct visualisation of the uterine cavity to treat polyps, submucosal fibroids, adhesions and septae.
Laparoscopy Treatment
Keyhole abdominal surgery for endometriosis, ovarian cysts, fibroids and tubal disease.
Endometriosis Treatment
Specialised management of endometriosis and its impact on fertility.
IVF Treatment
In Vitro Fertilization — often the next step after surgical optimisation of the reproductive tract.
Related Articles
Laparoscopy vs Hysteroscopy: Key Differences
Laparoscopy vs Hysteroscopy explained by Chennai fertility specialist Dr. Rukkayal Fathima. Understand the differences & which is right for you.
10 min read
Laparoscopy Cost in Chennai: What to Expect
Understanding laparoscopy cost in Chennai. Learn about diagnostic vs operative costs & factors affecting pricing. Expert guide by Dr. Rukkayal.
8 min read
Hysteroscopy: What to Expect
Learn about hysteroscopy in Chennai: procedure, recovery, cost, and benefits. Expert guide by Dr. Rukkayal Fathima.
9 min read
Laparoscopy: Is It Needed for Infertility?
Understand the role of laparoscopy for infertility in Chennai. Expert insights on diagnosis, benefits, and when to consider this surgery.
8 min read
Period After Hysteroscopy: What to Expect
Understand your menstrual cycle after hysteroscopy in Chennai. Learn about period delays, bleeding, and when to seek help.
7 min read
Ready to Get Started?
Book a consultation with Dr. Rukkayal Fathima about your treatment options
Book AppointmentBook Consultation
Consultation Booked!
Thank you for reaching out. Our team will contact you shortly to confirm your appointment.
Need urgent help? Call us